Invertebrates
with no true circulatory system (eg. earthworm) respond to an irritant by surrounding it with specialised cells (haematocytes) which then ingest it. If
the damage is very severe, the invertebrate simply rejects the injured portion
of its anatomy as a prelude to its regeneration. In higher animals such as
humans, the local reaction to injury is much more complex because of the
evolution of the circulatory system, and the disappearance of the kind of
regenerative powers seen in the earthworm.
The local
reaction to injury is called inflammation (from the Latin word inflamare meaning ‘to burn’. Four
cardinal signs signify inflammation:
·
Red
(erythema)
·
Hot
(heat)
·
Swollen
(inflammation)
·
Tender
(pain)
Given the extent
of disturbance, it goes without saying that there will undoubtedly be a loss of
function too. Some experts classify this as the fifth cardinal sign. Although
any tissue may suffer injury, inflammation is essentially the reaction to
injury of the living microcirculation and its contents. Although the
physiological mechanisms of inflammation haven’t changed over the years, the
theories and our understanding of its purpose and clinical significance has.
Current
Medical Thinking

Researchers are
linking inflammation and the inflammatory response to an ever-wider array of
chronic illnesses. Uncontrolled chronic inflammation is now considered a major
component of many widely occurring diseases, including asthma, atherosclerosis,
peripheral vascular disease, Alzheimer’s disease, cancer, ADHD, diabetes and
osteoporosis. This is in addition to the established pathophysiology of a range
of skin disorders, joint disorders, metabolic disorders and homeostatic
imbalances of inflammatory origin. Examples of current medical thinking include
novel approaches in the resolution of inflammation:
·
angiogenesis
and cancer (areas for Rx targeting)
·
autoimmunity
and RA
·
impact
of stress on inflammatory disorders of the GIT
·
chronic
inflammation and Alzheimer’s
·
biochemical
markers of inflammation esp. CRP (C-Reactive Protein). Others incl. adiponectin, MCP-1, CD40 ligand and Lp-PLA(2)
A certain amount
of focus these days seem to be on how active a process inflammation is and the
control of it. Also, there is considerable interest in the connection between
inflammation in one area of the body and others eg. gum disease and other
conditions.
Biochemical
Mechanisms & Principles of Inflammation
Inflammation is
the body’s response to injury (stimuli). These stimuli can constitute any of
the following:
·
physical
– damage to skin or other tissue or organ
·
chemical
– noxious chemicals/poisons
·
microorganisms
– toxins produced by them
·
immunological
– hypersensitivity reactions
Categorising the
type of inflammation is important as this will (to a large extent)
determine the treatment rationale. In short, inflammation is either acute
or chronic.
acute
- of short duration
- of short duration
- 4 cardinal signs on examination eg,
bacterial infection, flu, sprained ankle
chronic
- prolonged phase of inflammation (depending on nature of injury)
- prolonged phase of inflammation (depending on nature of injury)
- usually there
is a preliminary & sometimes recurrent acute episodes
- inflammation
& repair occur simultaneously with persistent
- suppuration
(pus formation) & ulceration leading to fibrosis (scarring) eg. chronic bronchitis, RA, IBD
Main
Features of Acute Inflammation
- dilation of blood vessels (heat & redness)
- increased vascular permeability (heat & redness)
- emigration of WBC along with inflammatory
exudate (swelling & pain)
Physiological
Significance of Inflammation
- Clot formation localises pathogens and
prevents loss of blood at the site if injury
- Inflammatory exudate contains antimicrobial agents
eg. Ab, complement
- Inflammatory exudate is continually drained
via the lymphatic so that pathogens and/or their toxins are drained into
the lymph nodes leading to the initiation of an immune response
Suppuration
Suppuration is an intermediate
situation with 2 main components:
- very large granulocytes ( a type of WBC that
incl. neutrophils) are summoned to the site of injury (usually by
chemotactic influence of certain bacteria such as S.aureus).
- the exuded WBC are killed in large numbers by the bacteria and their bodies liquefied by their own lysozymal enzymes to form a creamy, viscous fluid rich in lipids, proteins and nucleic acids – this fluid is known as pus. The mass of bacteria, dead, dying and liquefied WBC and surviving inflamed tissue is termed an abscess eg. when present in skin it is called a boil or sometimes a carbuncle if very large
Note: the painful abscess is the
price we pay for survival since it is an inevitable result of confining certain
dangerous bacteria to one part of the body rather than allowing them to
disseminate.
Inflammation
and the Nervous System (NS)
Many experiments
have shown that inflammation proceeds unmodified in the absence of any nerve
supply. This does not mean, however, that the NS is unable to influence the
inflammatory reaction. At the simplest level, the red flare that surrounds the
skin reaction to mild trauma (the triple response*) is abolished if
the sensory or vasomotor nerves are blocked or cut.
*
a simple way of demonstrating the early phases of acute inflammation
On a more
complex level, hypnosis, suggestion and emotional factors have been shown to
significantly influence the inflammatory response particularly, in the
sensation of pain. Equally, there is ongoing research interest in psychosomatic
disorders where emotional factors seem likely to play a major role.
Pain
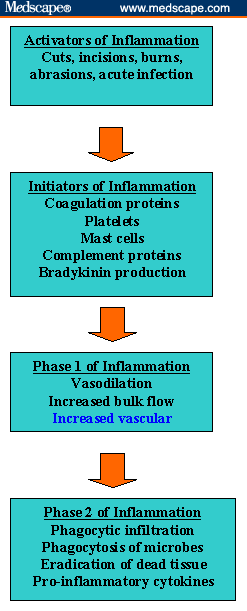 The heat,
redness and swelling of acute inflammation (due to vascular dilation and
increased vascular permeability) results in pressure on sensory nerve endings
by the exuded fluid and detected as pain. This is particularly the case if the
space in which it can expand is limited but it is partly due to the release of bodily
substances which stimulates these nerves. These substances are collectively
referred to as chemical mediators of
inflammation (see table below) and have wide-range actions.
The heat,
redness and swelling of acute inflammation (due to vascular dilation and
increased vascular permeability) results in pressure on sensory nerve endings
by the exuded fluid and detected as pain. This is particularly the case if the
space in which it can expand is limited but it is partly due to the release of bodily
substances which stimulates these nerves. These substances are collectively
referred to as chemical mediators of
inflammation (see table below) and have wide-range actions.
eg.
histamine, serotonin, kinins, prostaglandins are all linked to pain.
eg.
other chemicals liberated by nervous stimuli or cell injury eg Ach or K+ may
also be painful
Mediator
|
Main source
|
Histamine
Kinins (eg.
bradykinin, leucokinins)
Prostaglandins
(E1 & E2) & acidic lipids
Slow
reacting substances
Complement
components
Clotting
system components (fibrinopeptides)
Cytokines
|
Mast cells
or basophils
From blood
cell precursors by proteases and WBC
Polymorphonuclear
leucocytes, monocytes and basophils
Mast cells
and basophils
Derived by
activation of classical or alternative pathways
Blood and
tissue fluids
Lymphacytes
& macrophages (WBC)
|
Significance
of Pain
The survival
value to the host of pain is obvious as it sends a signal that there is injury/damage
and that part of the body needs to be favoured and rested. However, the reverse
is true if body function is limited because of the pain itself.
Hypersensitivity
The normal
acquired immune mechanisms perform a useful function in combating infection.
However, disadvantageous reactions can unfortunately occur at the same time.
eg. release of inflammatory mediators that,
whilst helpful in phagocytes serum Ab or complement to the site of infection,
can also cause damage to tissue cells.
Even cellular
immune reactions can result in the destruction of host cells. These
disadvantageous reactions are called hypersensitivity reactions or allergies. There are 4 types:
Type 1
IgE Ab attached to mast cells react with Ag (sometimes called allergen) and trigger the release of histamine, a slow-reacting substance of anaphylaxis and eosinophil chemotactic factor. This is the mechanism of many common forms of allergy eg. atopic allergy (hayfever, eczema, asthma), urticaria
IgE Ab attached to mast cells react with Ag (sometimes called allergen) and trigger the release of histamine, a slow-reacting substance of anaphylaxis and eosinophil chemotactic factor. This is the mechanism of many common forms of allergy eg. atopic allergy (hayfever, eczema, asthma), urticaria
Type 2
IgM or IgG Ab react with Ag (often a drug or microbial product) attached to tissue cells, such as WBC or RBC. This results in complement activation and lysis of the cell.
IgM or IgG Ab react with Ag (often a drug or microbial product) attached to tissue cells, such as WBC or RBC. This results in complement activation and lysis of the cell.
Type 3
IgM or IgG Ab form complexes with Ag and activate complement. Chemotactic factors and other inflammatory mediators are generated and tissue damage results. This is sometimes called immune complex disease and is responsible for vasculitis and kidney damage
IgM or IgG Ab form complexes with Ag and activate complement. Chemotactic factors and other inflammatory mediators are generated and tissue damage results. This is sometimes called immune complex disease and is responsible for vasculitis and kidney damage
Type 4
Sensitised T-lymphocytes (WBC) interact with Ag for eg. products of mycobacteria or sometimes even simple chemicals attached to body proteins. Lymphokines are released and can cause inflammation. These reactions are sometimes called delayed hypersensitivity responses or contact dermatitis when simple chemicals are involved.
Sensitised T-lymphocytes (WBC) interact with Ag for eg. products of mycobacteria or sometimes even simple chemicals attached to body proteins. Lymphokines are released and can cause inflammation. These reactions are sometimes called delayed hypersensitivity responses or contact dermatitis when simple chemicals are involved.
Note: genetic factors in allergy
must be considered so family history and previous exposure and events are
important clinical considerations. Other important points include:
- the IgE levels of normal individuals are low (approx. 0.1 mg/dL) and are controlled by a dominant gene. The higher the level of IgE, the greater the chance of allergic predisposisiton
- ragweed allergy is closely associated with the DW2 locus of HLA (Human Leucocyte Antigen). The HLA is the name of the major histocompatibility complex (MHC) in humans and contains a super locus (of which DW2 is one) contains a large number of genes related to immune system function
- immune hyperactivity particularly IgE response to a wide range of Ab is a feature if considering allergic individuals
Other factors include:
degree of exposure to Ag (allergens)
degree of exposure to Ag (allergens)
nutritional status of the
individual
presence
of chronic infections
acute
viral infections
Autoimmunity
Whilst
immunological responses to foreign agents are powerful, sometimes the body
starts to produce Abs against its own tissues. When this happens, there is
always a potent disease mechanism at play. There are two general categories of
autoimmune disease:
Organ
specific diseases: thyroiditis (Hashimoto’s Disease)
haemolytic
anaemia
pernicious
anaemia
Non-organ
specific diseases: SLE
RA
Between these
two extremes lie a number of conditions such as:
Juvenile
diabetes - Ab produced against
pancreatic islet Ag and WBC Ag
Primary biliary
cirrhosis - Ab produced against
mitochondria of various cells
Active chronic
hepatitis - Ab produced against smooth
muscle Ag and nuclei
Another strand of autoimmune
disease is extra-articular disease which is less well understood but can
include:
- anaemia
- rheumatic nodules
- vasculitis
- eye disease (eg. episcleritis)
- nerve lesions (eg. peripheral neuropathy)
- pericarditis
- pleurisy
- lymphadenopathy
- splenomegaly
- general malaise
Examples of associations
between HLA type and some diseases:
Disease
|
HLA
|
Frequency in %
|
|
Patients
|
Controls
|
||
Ankylosing Spondylitis
Reiters Disease
Acute Anterior Uveitis
Subacute Thyroiditis
Idiopathic Hemochromatosis
Psoriasis vulgaris
Coeliac Disease
Idiopathic Addison’s Disease
Insulin-dependent Diabetes
(IDD)
Myasthenia Gravis
Systemic Lupus Erythematosus
(SLE)
Multiple Sclerosis (MS)
Rheumatoid Arthritis (RA)
Hashimoto’s Thyroiditis
Pernicious Anaemia
|
B27
B27
B27
B35
A3
B14
CW6
DR3
DR3
DR3
DR4
DR3
B8
DR3
DR2
DR4
DR5
DR5
|
90
79
52
70
76
16
87
79
69
56
75
50
47
70
59
50
19
25
|
9.4
9.4
9.4
14.6
28.2
3.8
33.1
26.3
26.3
28.2
32.2
28.2
24.6
28.2
25.8
19.4
6.9
5.8
|
HLA = Human Leucocyte Antigen (or Major
Histocompatibility Complex/MHC)
Markers
of Inflammation
A number of
different biomarkers have been shown to be clinically relevant not only in the
onset of inflammation but also to predict risk (eg. CRP in CVD). This holds
significant potential for new therapeutic possibilities in conventional
treatment strategies. Other markers include:
o adiponectin
o monocyte chemoattractant
protein 1 (MCP-1)
o CD40 ligand
o lipoprotein-associated
phospholipase A(2) or Lp-PLA(2)
Conventional
Rx
Drug therapy
very much depends on the condition being treated, whether it is acute or
chronic and largely dictated by other considerations such as patient profile,
severity and response to initial treatment. Routine drug-based
anti-inflammatories fall into 2 major groups:
o NSAIDs (non-steroidal
anti-inflammatory drugs)
o Steroids-based anti-inflammatories
Both types of
drugs have adverse effects and depending on the duration of treatment, not all
patients respond favourably to long-term prescription without encountering
problems and/or complications as a consequence. It is this without doubt, that
patients most seek help from natural therapies and CAM
alternatives to either treat or manage a range of inflammatory conditions.
Homeostatic
Imbalance and Inflammation
The very nature
of inflammation means that homeostasis is significantly compromised and this
has profound and often devastating endocrine, metabolic, cellular and systemic
effects. Consequential effects can be addressed by a symptomatic approach
(clinical features) but a more holistic approach is very often necessary if the
cause and nature of inflammation is such that only a comprehensive examination
which considers all influences to the clinical presentation proves effective
especially in the long term.
New
Research & Novel Mechanisms
Whilst
inflammation may not be the causative factor in some widely occurring diseases,
it is now believed to contribute to disease progression, tissue dysfunction and
ultimately organ failure in these diseases. Resolution of inflammation was once
considered a passive process but in recent years, evidence has emerged that
this biochemically active process and more recent results have established some
of the chemical mediators involved. Elucidation of biochemical pathways
contributing to the resolution of inflammation has provided many new
anti-inflammatory targets and an opportunity for resolution-based pharmacology
for the treatment and prevention of inflammatory disorders.
Studies
examining the mechanisms of inflammation and the process of resolution (healing
& repair) leading to new therapeutic possibilities include the following:
· atherosclerosis
· acute inflammation
· endogenous anti-inflammation
· inflammation, healing & angiogenesis in the eye
· endogenous mediators
